DEATH BED
The story of Kelly Savage
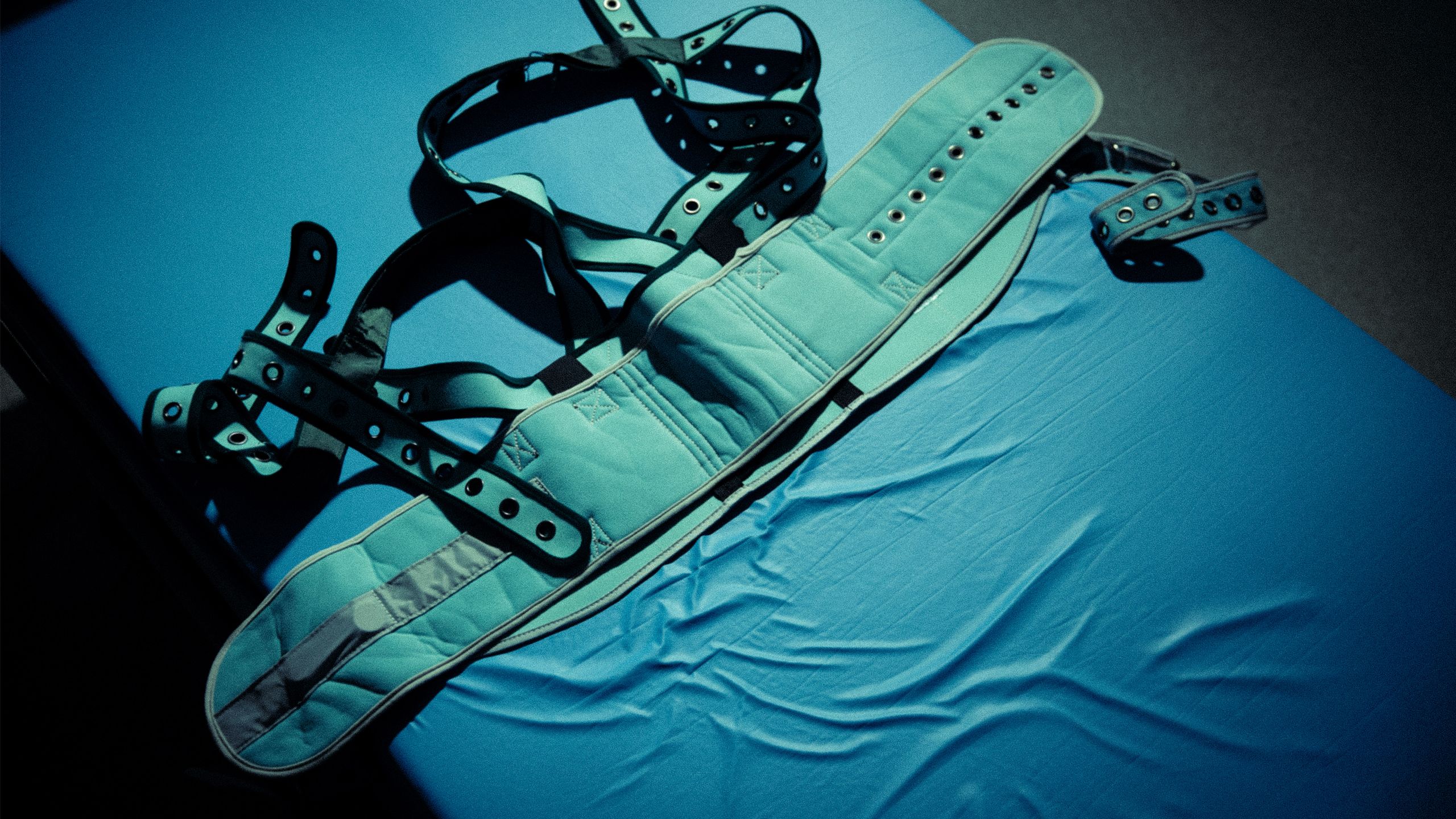
A young New Zealander entered a Japanese hospital in psychosis. He left braindead. His grieving mother is fighting for change.

Martha Savage doesn’t like to listen to music anymore. Most of the songs she used to enjoy seem to be about death. They make her too emotional now, she says. It’s been two years to the day since her 27-year-old son Kelly Savage died. The young Wellington man spent his final week in a coma, kept alive by machines. Before that, for 10 days straight, Kelly had been drugged and physically restrained - strapped to a bed at his wrists, ankles and waist. For around 240 hours, Kelly lay in bed in an adult diaper, isolated in a locked, windowless cell, inside a locked ward, on the second floor of a psychiatric hospital in Japan.
The Savage family firmly believe this long period of restraint caused Kelly’s death. One of the biggest risks of such a prolonged lack of movement is deep vein thrombosis, a condition where a large blood clot formed in the leg or pelvis breaks off and travels to the lung or heart, causing a blockage of blood or oxygen, which can lead to cardiac arrest.
An inconclusive post mortem means they will probably never know for sure if it was a blood clot that killed Kelly. A lack of cooperation from the private hospital that tied him down means their questions about why he was restrained for so long remain unanswered.

Yamato psychiatric hospital, where Kelly Savage was tied to a bed for 10 days.
Yamato psychiatric hospital, where Kelly Savage was tied to a bed for 10 days.
At first glance, Martha, a professor of seismology at Victoria University, seems stoic and almost clinical in her approach to her son’s death. She takes every opportunity she can to speak about it. She has travelled to Japan to campaign against the prolonged use of physical restraints in psychiatric hospitals twice since Kelly died on 17 May, 2017 - once to present a petition to Japan’s Ministry of Health, Labour and Welfare calling for a review of restraint use, and a second time to present an open letter addressed to Prime Minister Shinzo Abe, signed by 31 psychiatrists, calling for an international inquiry into the issue. In February, at the Japanese embassy in Wellington, about two dozen people watched as she gave a PowerPoint presentation. She showed little emotion as the enormity of her battle for change was revealed, slide by slide.
But the lack of emotion is a facade, and although Martha’s stoic determination is real, it’s also a coping mechanism; she likes to keep busy. Around her neck, she wears a silver pendant containing fragments of Kelly’s ashes. Everything reminds her of him - her students, people’s names, places he’s been. At work, her desktop image is Kelly atop Mt Fuji at dawn, fists in the sky, grinning. At the Savage family home in Karori, the walls are covered in photographs - weddings, birthdays, graduations. The largest of these is a silver-framed portrait of Kelly holding his niece. “He lives in here,” she says, gesturing to the room.

Kelly was an active, happy child, his mother says.
Kelly was an active, happy child, his mother says.
It’s in this room that Martha wells up when talking about her son’s death. She falls silent, removes her glasses and dabs her eyes with a tissue, puts them back on, then finishes her sentence. She refuses to give up the fight for justice for Kelly. She wants change in Japan. “We have to try to keep other people from the same fate.”
TIED DOWN
“We had no idea that it was a death sentence.”

In New Zealand, if a person dies in a psychiatric hospital, the death must be reported to the coroner and, by law, an inquest must be held. In Japan, there is no such law. When Kelly died after being restrained at Yamato psychiatric hospital, a private facility in Kanagawa Prefecture, there was no external investigation. In order for one to be held, the hospital’s doctors, nurses and management staff would have to report themselves to Medsafe, Japan’s medical accident investigation authority. Perhaps unsurprisingly, and despite repeated requests from the Savage family for the hospital to do so, Kelly’s death was not reported as being out of the ordinary.
In a letter to the family, as part of its reasoning for not reporting Kelly’s death, Yamato hospital denies having restrained the 27-year-old for 10 days, saying he was released “from time to time and only restrained when necessary.” The section of his medical records that have been viewed by RNZ contradict this statement; they say that Kelly was restrained the entire time he was in hospital.

The prolonged use of mechanical restraints in psychiatric care - like the ones used on Kelly - is illegal in Japan, except under extreme and unavoidable circumstances; if the patient is a risk to themselves or those around them, for example. Kelly was tied to a bed at Yamato hospital for 10 days. The straps were so tight they left marks on his body. His family say he was so heavily sedated he had trouble breathing, eating and speaking. He had a high temperature and was being treated with antibiotics. Was he really in such a state that he posed a risk to himself and others for the 240 hours he spent at Yamato psychiatric hospital?
Kelly’s older brother Patrick Savage says no. He was with Kelly when he was committed to the hospital by two psychiatrists, one of whom was the hospital’s director, Kazuhiko Ishii. It was 30 April, 2017, a Sunday, about 3pm.
Kelly’s mental health had begun to deteriorate in early 2017, so on 25 April he travelled from southern Japan, where he worked as an English teacher, to Yokohama to stay with Patrick, an associate professor in the faculty of environment and information studies at nearby Keio University. Kelly needed some time out to get back on track. But rather than getting better, he got worse. Patrick says his behaviour became manic.

Patrick Savage thought he was helping his brother by getting him hospitalised.
Patrick Savage thought he was helping his brother by getting him hospitalised.
“At one point he just suddenly jumped up and ran outside. I followed him and he ran downstairs, he grabbed some stuff off the shelf of the convenience store and then he put it back. He was darting round, acting really bizarre. I managed to get him to come back up to the apartment and get him back into his room, but he just seemed like he was getting more and more … not in a good place.”
By the morning of 30 April, Kelly was screaming, moving furniture and pulling up rugs, and no one - not Kelly, Patrick, nor their father Mike, who was visiting from New Zealand at the time - had slept for close to 24 hours.
When Patrick called an ambulance service for help, they refused to come, so as a last resort, he called the police. When they arrived, Kelly tried to escape and it took eight officers to restrain and handcuff him. Once he was in custody, Patrick says he calmed and eventually he was taken to Yamato psychiatric hospital. “He was still paranoid, but he wasn’t trying to struggle.”
Kelly was put in a wheelchair and taken to a locked ward on the second floor of the hospital. When he was wheeled into a three by five metre room, Kelly complied with instructions, got out of the wheelchair and lay down on the bed. Patrick signed a form consenting to pay for pyjamas and an adult diaper. Kelly would need it, a nurse said, telling Patrick he would be in the bed for 'quite a while.' A wide belt made of fabric similar to that used in bullet proof vests, and fastened to the bed, was strapped tight around Kelly’s waist and secured with metal pins. Similar restraints were placed around his ankles and wrists, preventing his ability to move almost entirely. Patrick and Mike thought they were helping Kelly out by putting him in hospital. “We had no idea that it was a death sentence,” Patrick says. The concrete room, which contained only the bed and a metal toilet bowl, was locked, and Kelly was left alone.
Patrick was allowed to see his brother briefly two days later, on 2 May, but then not again until 8 May. In the meantime he called the hospital daily. “I would ask how he was doing and ask if they’d taken the restraints off. They kept saying no.”
Did Kelly’s behaviour in hospital mean staff had no option but to restrain him? Yamato hospital has repeatedly refused to answer RNZ’s questions about his death, as has the hospital’s lawyer. The hospital also refused to release Kelly’s medical and nursing records to the Savage family until the evening of 19 July, 2017, immediately after Martha and Patrick held a press conference with Japanese media, and more than two months after Kelly died.
These records tell a contradictory and suspicious story. At 1.47pm on 1 May, they read: “Drowsiness is ongoing. There is no restless behaviour.” But by 4.30pm things have apparently changed dramatically: “In a state of psychomotor excitation, with significant restlessness, hyperactivity and explosiveness. There is sufficient risk of the patient being injured if not treated.”
On 5 May, at 2.30pm, Kelly is described as being drowsy, and snoring loudly. “If spoken to, the patient very occasionally replies with ‘yes’. Otherwise the patient responds by nodding. Is not trying to get up and there is no restless behaviour.” But two hours later, the exact same comment from 1 May reappears in his notes: “In a state of psychomotor excitation, with significant restlessness, hyperactivity and explosiveness. There is sufficient risk of the patient being injured if not treated. The patient’s trunk and limbs are restrained.”

On 8 May, two days before his heart stops, Kelly’s records mismatch even more dramatically. At 8.28am staff observed the following: “Appearance at breakfast time with full assistance, ate two thirds. The patient occasionally choked on liquids but is able to eat if time is taken. When the staff speak to the patient, the patient communicates well and sometimes smiles. The patient wanted to try to brush their own teeth so the patient did it slowly with staff present. The patient said ‘Thank you again this morning’.” Two minutes later, at 8.30am, the same statement seen in previous days’ notes appears: “In a state of psychomotor excitation, with significant restlessness, hyperactivity and explosiveness. There is sufficient risk of the patient being injured if not treated. The patient’s trunk and limbs are restrained.”
The records beg the question, did Kelly’s behaviour veer wildly from moment-to-moment? Or were some staff making truthful observations, while others copied and pasted the same line into his records again and again, knowing those three sentences legally justified keeping Kelly restrained?
The contradictory statements are evidence that someone in the hospital is lying, says Yokohama-based human rights lawyer Nobuo Sasaki, who has worked with the Savage family. But he says this evidence is not enough to trigger an independent investigation into Kelly’s death; the Savage family would have to sue the hospital to see justice, and even then, victory is unlikely. (The family has decided against getting involved in a drawn out legal battle with the hospital.) “The cases that patients have won against psychiatric hospitals are few,” Sasaki says, “because the governments and people of Japan support Japanese psychiatry.”
The United Nations’ Committee Against Torture has repeatedly raised concerns about Japanese private psychiatric hospitals’ and psychiatrists’ power to issue detention orders, and the lack of sufficient judicial control over this process. In 2007 the committee also noted concerns around “management of private mental health institutions” and management of complaints by patients relating to “acts of torture or ill treatment.”
KATHRYN MORRIS
“She chose death.”

As a teenager, Kathryn Morris’ glossy brown curls and wide smile reminded her mother Marilyn Morris of the actress Kate Winslet. But when Marilyn flew from Auckland to visit her cherished eldest daughter at a psychiatric hospital in Japan, Kathryn’s eyes were sunken and her complexion was sallow. “They have deadened my brain,” she told her mother.
It was 27 October, 2003, five days after Kathryn had been involuntarily admitted to Narita Red Cross Hospital during a severe psychotic episode. When Marilyn arrived, her then-27-year-old daughter had just woken from a four-day stupor. She was loaded with antipsychotics, restrained at her waist, ankles, and wrists, wearing a diaper, a urinary catheter and blue uniform pyjamas.
Marilyn says she understood that Kathryn needed to be sedated, because she was exhausted. “Her overwrought brain needed to recover.” But she did not think it was necessary for her daughter to be tied down. Strong sedatives, Marilyn says, ought to have been enough.

Kathryn had been living in Japan only three months when she became manic - she didn’t sleep for 10 days - and was hospitalised. The young teacher was working at a school in Hamamatsu, a coastal city south of Tokyo. At 24, Kathryn had been diagnosed with bipolar disorder. Her mother, a registered nurse, says Kathryn never accepted her illness, and mostly refused to take the lithium she was prescribed.
Inside the locked ward at Narita Red Cross Hospital, Kathryn’s room was small and austere. A clock hung on one dull, white wall, and on another the locked window was so opaque that nothing was visible through it. Marilyn noticed a calendar tacked to the wall, and inside it found Kathryn’s handwriting, scrawled in pencil across the pages, forming the sentence, ‘Get me out of here’, over and over. “It was heartbreaking,” Marilyn says.
Kathryn’s restraints were removed after four days in hospital and by 3 November, she was home in New Zealand, attending regular appointments with a psychiatrist in Auckland, where the family lived. But by 5 January 2004, she was back teaching in Japan.
About two weeks after Kathryn’s abrupt departure from the family’s Castor Bay home, Marilyn was horrified to find her daughter’s full bottle of lithium tablets in the bathroom cabinet. “Do not stop taking the medicine,” the label read.
By May 2005, Kathryn was again severely unwell - telling her mother of recurring nightmares and a terror of returning to New Zealand when her teaching contract expired in August. She feared rehospitalisation - believing she would be given a lobotomy, and would die alone in her hospital bed. When Marilyn asked Kathryn how much lithium she was taking, she told her half the prescribed dose. The truth, Marilyn later found out, was none at all.
It was autumn in Auckland, and Marilyn still remembers the clothes she was wearing on the evening of 6 May, as she sat down at the kitchen table to read the newspaper; brown corduroy pants, a red t-shirt and a pale green jersey a friend had knitted for her. It was about 9pm when she heard a knock on the door. Her husband Ian answered. It was two police officers. They asked Marilyn if she was Kathryn’s mother, and whether Kathryn was in Japan. On Thursday 5 May, at 10.43pm, they said, she had stepped into the path of an oncoming train.
Kathryn’s alternative, Marilyn says, was readmission to a Japanese psychiatric hospital, and restraint. “She chose death.”
KELLY’S DREAM
“He was a very bright character.”

Martha tells the story of Kelly’s birth with a smile. He was so eager to get out of the womb that he broke his own shoulder. Martha had planned to get an epidural, but she didn’t have time.
As a baby, he was active - more interested in watching people than eating. When Martha nursed him, he’d stay still a few minutes then move away, look around. He started walking at 10 months, and as a toddler he loved to throw rocks into a ditch behind their home in Reno, Nevada. He and Patrick were always very close.
Kelly was 5 when the Savage family moved to Wellington. He started at Karori Normal School straight away. “I actually wish that we’d waited a year," Martha says. “He really didn’t like to sit. He didn’t want to sit down for six hours a day.” Kelly was a happy child. He loved people - and everybody seemed to love him back. He loved sport - cricket and basketball were his favourites - and he loved Japan.
When Kelly was about 9, the Savage family hosted their first Japanese exchange student. It became an annual tradition thereafter and Patrick says the home was always filled with Japanese guests and culture. At Onslow College, the brothers both studied Japanese and went on exchange programmes to Japanese high schools. At Victoria University, Kelly studied psychology and Japanese. His dream, Martha says, was to teach English in Japan through the JET (Japan Exchange and Teaching) programme once he graduated.

Martha, Kelly and Mike Savage.
Martha, Kelly and Mike Savage.
After Kelly finished high school, depression began to set in. Martha says he was good at keeping it secret. “I remember the doctor calling us in and … Kelly had just told him how depressed he was … That was the first we really realised. He really put on a good face, so, like, his friends never knew ... I remember one time when Kelly was still in the middle of a terrible depression and one of his friends told me, ‘Oh, Kelly always looks so happy, always seems so happy’ and I’m like, ‘What? Kelly? Happy?’ because at home he was really - he couldn’t get out of bed.”
In 2012 his depression worsened and he was hospitalised in Wellington for several weeks. Kelly began taking lithium, but his family say a diagnosis was never clearly established. It took him time to recover, and occasionally he relapsed, but in May 2015, he graduated with his degree and in July, he got his dream job as a JET teacher.
In Japan, Kelly worked for the Shibushi Board of Education in Kagoshima prefecture. He rotated between eight different schools in the area, but his favourite was Harada Elementary, where he taught English to primary school pupils. “Every time he was here, he was all smiles. He was a very bright character,” Yanagita Nozome, a teacher at the school remembers. He treated the students with respect, as equals, and they reciprocated. “They loved him.”

Kelly's former students at Harada Elementary School.
Kelly's former students at Harada Elementary School.
His students still talk about “Kelly sensei” with fondness. In the schoolyard, filled with clusters of tiny flowers that cascade from raised gardens like pink ice cream sodas, they reminisce. He told them that in New Zealand at Christmas time, Santa would be surfing, and taught them songs in English. There was the time it snowed in Shibushi - a rare occurrence that far south - when Kelly took them outside to make snowmen. There was the ‘fruit salad’ game - a cross between musical chairs and tag, and the time his family visited and taught a class about Halloween. The kids still remember some of the scary things they learnt about that day - they call them out: “Ghost! Bat! Witch! Devil! Spider! Mummy!” One of the girls dressed as a witch, and Kelly dressed as Yoshi - the dinosaur from Super Mario Brothers - in a green onesie.
Kiyoshi Miyata, a teacher and artist from Shibushi, recalls the first time he saw Kelly, a tall, pale westerner with a scruffy mop of curly brown hair, sitting in a local pub one evening, eating breakfast food - rice, miso soup and an omelette - for dinner. “I asked, in English, ‘Where are you from?’” To Miyata’s surprise, Kelly’s response was in perfect Japanese: “I’m from New Zealand ... Do you like chicken nanban?” Miyata did like chicken nanban. They ordered and ate the dish together, and immediately became friends.
Kelly and another friend Clay Xiong, a JET teacher from Minnesota, lived in neighbouring apartments in a multi-storey block, close to the waterfront, above a Taiwanese restaurant in the centre of town. Xiong recalls that on their first day on the job, they were expected to dress in a suit and tie, and make speeches. “I was super nervous because my Japanese is not that great,” he recalls. “I’m about to leave for school when my doorbell rings.” It’s Kelly, asking Xiong not only if he can borrow a tie, but if Xiong can tie it for him. “I was in middle school when I learnt to tie a tie … Kelly was a year older than me. So that was the beginning of a strange and wonderful friendship.”
When Martha, Patrick and Mike visited Kelly in Shibushi, in early November 2016, they had a wonderful time. But in the back of her mind, Martha worried about Kelly, as she had done since he was first hospitalised in 2012. He took his medication irregularly, and would go in and out of bouts of depression. Martha believes he stopped taking his lithium altogether around January 2017.

The Savage family visiting Harada Elementary School.
The Savage family visiting Harada Elementary School.
None of Kelly’s friends in Japan knew he was unwell. He seemed so happy. In Shibushi, he loved to run in a large, grassy park overlooking the port’s candy-striped cranes, or to visit Daguri Beach, where sea turtles laid their eggs in the summer. On clear days, he would drive up to Kokusai no Mori - a forested area in the hills above Shibushi, where cherry trees blossom in spring, and violets stretch their way out of shady nooks between stepping stones smoothed by thousands of feet.
In the wintry months of early 2017, it would already be dark outside when Xiong came home from work about 6 or 7pm. He would notice Kelly’s car parked at their building, and look up to see his apartment lights already off. He would wonder if Kelly was out, or home, if he was awake, or sleeping. The last time Xiong saw Kelly, it was spring, just before the city’s biggest festival. “I asked him if he was going. He said, ‘If I can’.” Kelly told Xiong he wasn’t feeling well and was going to stay with Patrick for a while.
“I wasn’t really sure what he meant, and all he said to me was, ‘I went to a hospital in Kanoya’, which is the next town over, and he said, ‘They couldn’t help me so I have to go somewhere - to a bigger city, so I decided Tokyo.’ I kind of got the feeling that maybe it could have been serious, but he didn’t want to talk about it … I figured it was private, I didn’t want to pry, so I said, ‘Have a nice trip and we’ll see you when you get back. Take care and have fun in Tokyo with your brother. ’”
A BROKEN SYSTEM
“They are profiting from care, but ignoring patients’ human rights.”

Japan’s mental health system stands out among OECD countries for all the wrong reasons. While other countries have, for decades, trended towards deinstitutionalisation and community care, about 290,000 in-patients occupy the 330,000 beds in Japan’s psychiatric hospitals. More than 90 percent of the country’s approximately 1200 psychiatric hospitals are privately owned.
Japan has the highest number of psychiatric beds per patient in the OECD - 2.6 per 1000 people (the second highest country, Belgium, has a rate of 1.4, the OECD average is 0.7 and New Zealand’s rate is 0.3), and psychiatric hospital expenditure makes up 76 percent of the government’s total mental health budget.
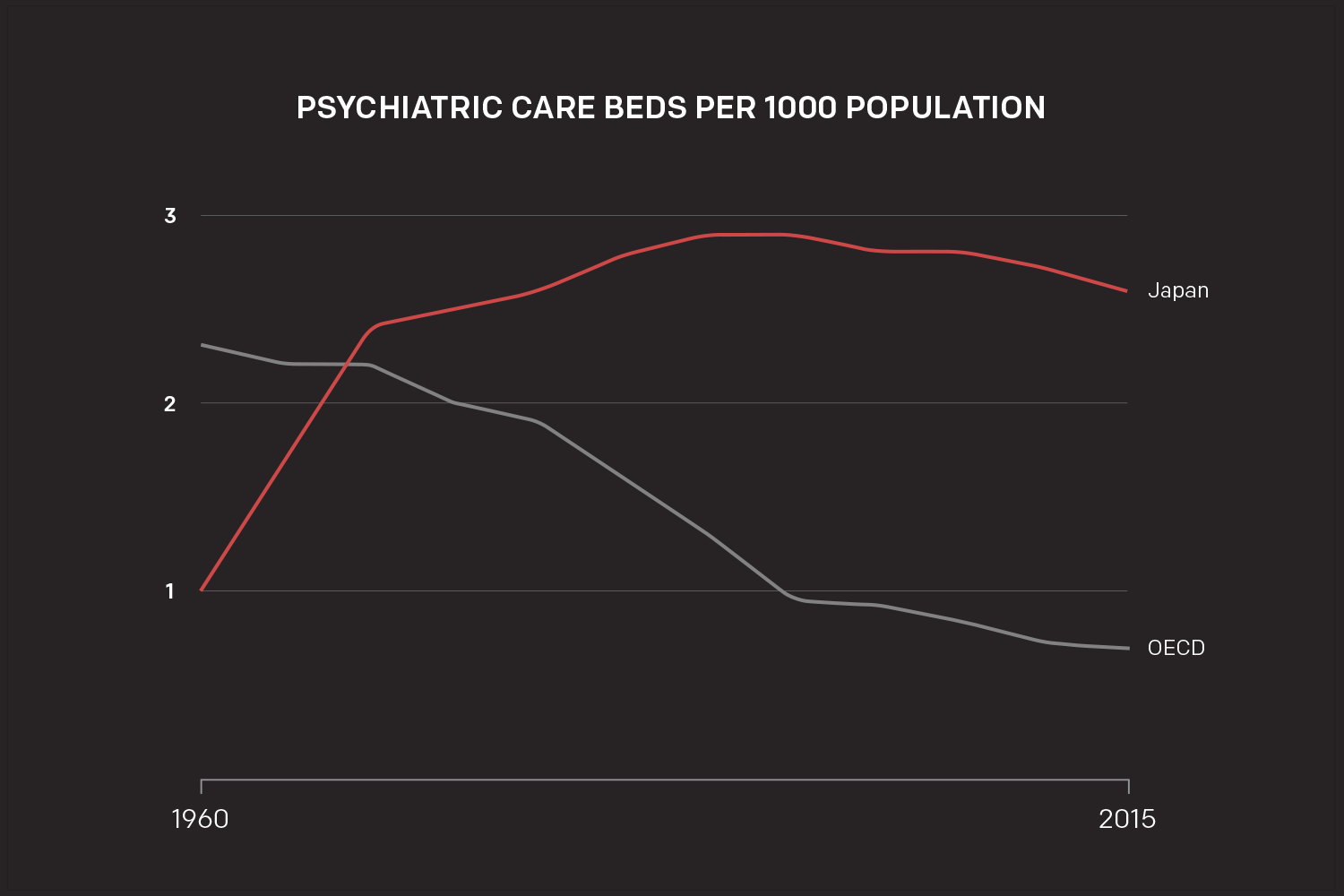
Source: MHLW, OECD.
Source: MHLW, OECD.
In addition, patients admitted to psychiatric hospitals in Japan tend to remain in hospital an extremely long time compared to other countries. In 2011, 65 percent of patients (about 182,000 people) who were admitted to psychiatric hospitals stayed more than a year, and the overall average length of stay was 298 days. The OECD average is 36 days. In October last year, an investigation by newspaper Mainichi revealed that 1700 people had been kept in Japanese psychiatric hospitals for more than 50 years.
Journalist Yukiko Okuma writes about and campaigns against the use of restraints in Japanese psychiatric hospitals. She says private psychiatric hospitals benefit from Japan’s universal health insurance scheme, which pays for patients’ lengthy stays. “[Psychiatric hospital] owners want to make money from patient care. So the reason CEOs don’t want to discharge patients is that they want to get money.” Joukei Ariga, a psychiatric nurse and spokesman for Osaka Center for Mental Health and Human Rights - a support group for patients and their families - also says that private hospitals put money first. “They are profiting from care, but ignoring patients’ human rights. Our mission is to change this situation.”
In a scathing 2015 OECD report on the quality of health care in Japan, the mental health care system is described as lagging behind other countries. “The difficult reality for the Japanese mental health system is that if high quality mental health care for severe mental illnesses is to be firmly established, inpatient beds will have to be reduced significantly and some psychiatric hospitals will have to close.”
But the closure of psychiatric hospitals in a country where 90 percent of them are private would be a major challenge for the Japanese government. Hospitals are represented by the powerful lobby group the Japan Psychiatric Hospitals Association, whose influence extends into the highest levels of the Japanese government. Its president, Dr Manabu Yamazaki, is said to be close friends with Prime Minister Shinzo Abe, and the cover photo on his Facebook profile shows the pair sitting with their arms around one another. Both Yamazaki and the association declined or ignored RNZ's multiple interview requests.

Prime Minister Shinzo Abe, left, with Manabu Yamazaki.
Prime Minister Shinzo Abe, left, with Manabu Yamazaki.
Okuma says the association lobbies the government and makes donations to politicians, and this accounts for the lack of political drive to change policies that would improve the system for its users. In a 2012 collection of essays on Japan’s mental health care system, the association is blamed for the country’s lack of meaningful reform. “Drastic changes in current mental health systems could seriously affect and damage their hospital management, so changes need to come gradually, which is the basic idea of the association.”

Ministry of Health, Labour and Welfare, Tokyo.
Ministry of Health, Labour and Welfare, Tokyo.
In 2011, Japan’s Ministry of Health, Labour and Welfare, which oversees laws governing healthcare, announced it had selected 24 psychiatric hospitals as part of a trial programme which required them to remove at least 10 percent of their beds within five years. The hospitals, 17 of which were private, were also required to set up teams to help care for patients released into the community. The Ministry has not said how many beds were removed under this programme.
THE WRESTLER
“There’s no way to heal people by isolating or restraining them.”

There are no other countries where people in psychiatric hospitals are treated the way they are in Japan, says Toshio Hasegawa, a stocky man with rumpled black hair and cauliflower ears - a remnant from an early career as a professional wrestler. Hasegawa knows of 10 people who have died in the last six years after being restrained in Japanese psychiatric hospitals.
Now a professor of health sciences at Kyorin University in Tokyo, Hasegawa has previously worked in those hospitals, and takes a special interest in the use of mechanical restraints in mental healthcare. He’s written the book. Alongside Martha Savage, he fronts the Alliance Against Physical Restraint in Psychiatric Care - a group campaigning to ban the use of restraints for more than 24 hours in a country where patients can be tied down for years.
Hasegawa’s small office is in stark contrast to Kyorin University’s new and bafflingly clean campus. Along one wall, a bookshelf is bursting with volumes, their coloured spines freckled with bold, black Japanese script. Dividing the room down the middle is a pinboard covered in newspaper articles and documents that overflow onto the adjacent wall.
Hasegawa sits at a narrow table in the room’s centre, which is squeezed between stacks of paper. He leans back in his chair with a hand placed at each end of a small mountain of books marked with pink and yellow post-it notes. His brows wiggle when he speaks, punctuating his slow, thoughtful sentences. Mostly, he speaks in numbers.
There are, for example, the 12,528 restrained patients that were counted on one day, 30 June 2017, in Japan’s psychiatric hospitals (the annual 30 June survey is overseen by Japan’s Ministry of Health, Labour and Welfare). Then there are the 1756 people who were both isolated and restrained on that same day - not long after Kelly Savage’s death.

A restraint demonstration on journalist Hiroko Aihara.
A restraint demonstration on journalist Hiroko Aihara.
In many other countries, mechanical restraints are used in psychiatric care, but in moderation. Hasegawa says that on average, in Switzerland, patients are restrained for 48 hours; in Finland and Germany, the average time is 9.6 hours, while California’s average time is 4 hours. But in Japan, statistics on restraint times are not collected by the Ministry of Health, Labour and Welfare, the government department that oversees Japan’s mental health laws. So Hasegawa has done the research himself. After surveying 11 psychiatric hospitals, he found the average term of restraint was 96 days, with a median term of 19 days. The maximum time a person had spent in restraints was 1096 days; that's three years.
“They’re not treating patients as humans, they’re treating them like dangerous animals,” Hasegawa says. “This is not a way to care for people. There’s no way to heal people by isolating or restraining them.”
So why do they do it?
According to the Japanese Association of Psychiatric Hospitals, it’s because of an increase in people suffering from sudden bouts of acute mental illness. But the number of patients in psychiatric hospitals has actually slowly decreased since it peaked at 349,052 in 1991 (there are currently about 290,000 inpatients in Japan’s 320,000 psychiatric hospital beds).
Hasegawa is not convinced that this is the reason. “I wonder,” he says, “is it really possible for the number of people with serious mental illness to increase so suddenly?"
He offers an alternative explanation. “I think that it’s not that more people have severe mental illness, but that some institutions start by putting people in restraint.” Hasegawa suggests that some of the patients that are being restrained on admission to hospitals do not require restraint at all.
Hasegawa was there when Martha and Patrick Savage went public about Kelly’s death, at a press conference in Tokyo on 19 July, 2017. It was the first time identifiable victims of Japan’s broken mental healthcare system had spoken out. Japan is a country where a powerful stigma keeps the mentally ill confined to bedrooms or locked in hospital wards, separate from the community and even their own families, who are often not allowed to visit them. It also has one of the highest suicide rates in the OECD. Hasegawa says those who speak out about mental illness often face criticism. He himself is considered by some who work in psychiatric hospitals to be naive and idealistic.
But since the Savage family’s press conference, Hasegawa has been inundated with calls from families of people restrained in some of Japan’s 1200 psychiatric hospitals. This includes the parents of 40-year-old Kazuya Ohata, a carpenter from Ishikawa prefecture. Ohata was diagnosed with schizophrenia as a 25-year-old. In early December 2016 he was admitted to a Japanese psychiatric hospital. Despite desperately trying, his parents were not allowed to visit him, and after being restrained for seven days, he was found dead in the space between his bed and the wall. An autopsy found the cause of his death was a pulmonary thromboembolism, the result of deep vein thrombosis. His parents are in the process of suing the hospital where he died, and have held a press conference speaking out against the use of restraints.

Kazuya Ohata (right,) aged 23, with his younger brother Takashi.
Kazuya Ohata (right,) aged 23, with his younger brother Takashi.
Hasegawa says the Savage and Ohata families speaking publicly about their loved ones’ deaths is a good starting point, but there is a long way to go before there is change. In a country where conformity is greatly valued, speaking out against the system is frowned upon. “Compared with other countries, it is very difficult for Japanese people to take legal action against the government, as it will be viewed by others as a betrayal,” he says. “Japanese people see the government as a parent. So if a person sues the government, they are betraying their parents.”

It’s an uphill battle. The results from 2018’s 30 June survey have not yet been released by the Ministry of Health, Labour and Welfare - many of the copies Hasegawa obtained through Japan’s freedom of information laws have been fully redacted. (An MHLW spokesman says 2018 survey results are still being tallied.) In October last year, the head of Japan’s Association of Psychiatric Hospitals said its member facilities - close to 90 percent of all psychiatric hospitals in Japan - would not participate in this year’s 30 June survey, due to concerns about patient privacy. But Hasegawa says the survey information that has been released in the past is generic - like the number of doctors, nurses, occupational therapists, and public telephones on each hospital floor - and does not put patient privacy at risk.
And so, in a way, Hasegawa’s wrestling career continues. The large cellphone he keeps in the breast pocket of his crisp white shirt will continue ringing as long as people in need of kindness and compassion are tied to their beds and left there.
In the last few days of his life, Kelly’s hospital records reveal that he asked to see his brother several times. But because of Golden Week - a series of public holidays in Japan - Patrick and Mike were not allowed to visit between 3 and 7 May. Hospital staff had initially told them that patients in the locked ward could not have visitors at all, but an exception was made allowing them to see Kelly for 20 minutes a day after the holiday period - on 8, 9 and 10 May.
Click here to watch a video about Kelly Savage
“He was really happy to see me,” Patrick says. “The main thing he wanted to tell me was he was gonna be fine, 'don’t worry about me', 'don’t get too worked up about this stuff'. He wanted me to focus on my own life,” Patrick says. “That was when he was better - he seemed pretty out of it most of the time. He seemed really heavily medicated, so he had trouble talking. His tongue seemed thick, and he had trouble making words. He didn’t seem like he could get up even if he wasn’t tied to the bed.”
Kelly was fed mostly by IV, and was sedated with drugs like rohypnol and levomepromazine. He was paranoid, telling his brother the hospital food was poisoned, and that staff were trying to kill him. Martha spoke to him once via Skype, around 9 May, before she flew out for Japan 36 hours later. She says Mike and Patrick weren’t supposed to use cameras in the hospital, but they did it anyway. “At the beginning he was good, he talked to me but then he was kind of out of it and he was breathing hard, breathing very difficult.” Kelly’s breathing - a kind of struggled snorting, even when he was awake - reminded Martha of the way her father breathed when he was dying.
His medical records on 8 May say Kelly was “snoring continually”. The nurses, Martha believes, had questioned whether this was normal, and had moved him to a room closer to the nursing station. But Kelly’s doctor told Patrick that it was nothing to worry about. On 9 May, his medical records say he was “lower jaw breathing” - the type of breathing commonly observed in people close to death. On 10 May, Kelly ate breakfast and struggled to drink some tea. He ate half his lunch, with help, and was visited by Patrick. His diaper was changed, and he ate half his dinner, again with help from hospital staff. He remained restrained until a “sudden change” noted in his records finally led to the removal of his restraints. This “sudden change” was likely the massive cardiac arrest Kelly suffered at 9.25pm.
Dread hit Patrick when he saw he had five missed calls on his phone. After their daily 20 minute visit to Yamato psychiatric hospital, he and Mike had gone to an onsen - a Japanese hot spring that the brothers used to go to together. Upon calling the hospital back, Patrick learnt that Kelly had been rushed to a general hospital. “I asked if he was alive and they said, ‘I can’t say.’" He remembers the agonising, hour-long taxi ride to the hospital, not knowing whether Kelly was dead or alive. “It was just the worst time of my life.”
Kelly was wheeled past them just as they arrived at the general hospital. He was attached to a monitor, and Patrick and Mike saw there was a heartbeat. Not knowing how long Kelly’s heart had stopped for, and given his age and lack of history of heart disease, they figured he would be okay. They were wrong.
“After what felt like a million years, the cardiologist called us in and told us that his heart had stopped for 50 minutes … I didn’t know the details of these things, but that sounded like way too long.” Patrick says. “And, of course it was.”
When Kelly’s heart stopped, Martha Savage was preparing to board a flight to Tokyo. She had decided to wait a few days before travelling to Japan to avoid the public holidays so that she could visit Kelly in hospital, a decision she now regrets. Martha had assumed it would be just like the time Kelly was hospitalised in Wellington - it would take time, but he’d recover. She thought he was safe in hospital. It didn’t occur to her that it could lead to his death.
Patrick and Mike decided it was best not to tell Martha about Kelly’s cardiac arrest before she got on the plane. But when she touched down at Narita Airport in Tokyo, a barrage of messages popped up on what felt like every app on her phone. Patrick and Mike were at the airport to meet her. She was perplexed, as it was an almost four-hour round trip from Yokohama, and she usually took the bus to Patrick’s apartment. “I had a worry that there was something wrong. And then they came … and I saw their faces…”
Patrick and Mike sat Martha down and told her what had happened. Kelly’s heart was beating. He was attached to machines, there were tubes everywhere, his body would be cooled to induce a coma. “They were telling me that he might still be alive, we don’t know, his heart’s still beating but they didn’t know whether he was going to stay alive or not. Yeah. That was it.”
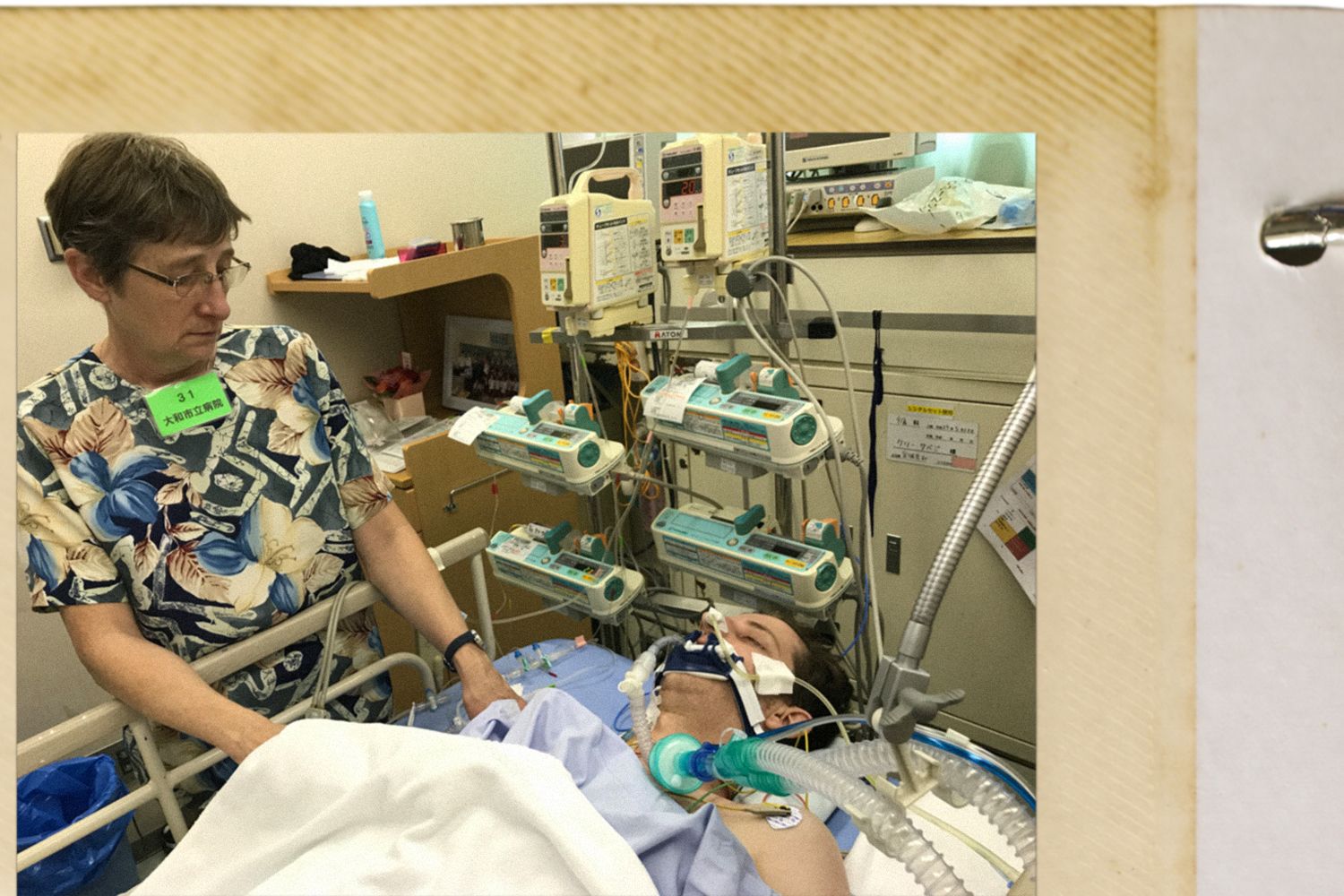
They put Martha’s luggage in a train station locker and headed to the hospital. Kelly looked like he was dying, Martha says. The family spent the next seven days at his bedside, waiting for him to regain consciousness. They tried talking, singing and playing music to him, but he never responded. Eventually, Patrick says, it became clear that Kelly was not going to wake up, and the waiting for a response turned into waiting for his brother to die. At some point, a cardiologist at the hospital told the family Kelly’s cardiac arrest may have been due to a pulmonary embolism - a blood clot blocking an artery in the lung. Such clots are commonly the result of deep vein thrombosis, which can be caused by prolonged immobility.
The news that the restraints Kelly was held in may have caused his death filled the Savage family with horror, grief and guilt. Could they have done something to remove them sooner? If they had acted differently could they have saved his life? After what seemed like forever, Kelly’s heart stopped beating on 17 May. It felt like a mercy. The Savage family washed his body, held an intimate memorial service, and watched as his casket was engulfed in flame.
The evening that Kelly’s friends in Shibushi learnt that he was unlikely to regain consciousness, they met in Xiong’s apartment, shared memories and tried to remain positive. But lying in bed that same evening, after everyone had gone home, Xiong saw a message from Patrick saying Kelly had died. He found his friend’s death hard to accept. It had been so sudden. Kelly’s car remained parked downstairs, where it always had been, and where Xiong still saw it every day. It felt to him like Kelly would still come back.
After the funeral, Xiong helped the Savage family clean out Kelly’s Shibushi apartment. “It was quite a mess,” Xiong says. “There were lots of Red Bull cans everywhere. Pat found like ¥ 20,000 ($277) in change just lying around. So Kelly bought us dinner that night.” Amongst the spare change and cans were piles of basketball magazines and books with Kelly’s name scrawled across the inside page in scratchy, childlike script - To Kill A Mockingbird, Crime and Punishment, For Whom The Bell Tolls, Catch 22, Kafka on the Shore, East of Eden. The books now live in Kelly’s friends' home - a reminder of the charismatic New Zealander with the Lion King tattoo on his shoulder, that is now on his headstone too.

When she heard about Kelly’s death, Harada Elementary School teacher Yanagita Nozome cried, and Kelly’s students there did too. “The only thing we could think to do was to write a letter to thank him for everything, so that’s what we did. The students put their hearts into the letters they wrote to him.”
To Kelly-sensei in heaven:
You taught me
All kinds of English
The days and the weather
Numbers and colours
Fruits and vegetables
Always with a kind smile
You were such a great teacher
You made me love studying English
Please watch over me from heaven
I will work hard because of you
- by Kelly's student Sakura Eno
GAIATSU
“Japan doesn’t change by itself, it changes by pressure from the outside.”

Kelly’s headstone is in a cemetery overlooking a park where he loved to play sports. Bushes covered with pink and white roses, thick like dense scribbles, tremble in the Wellington bluster. It’s bright, and Martha squints as she kneels down and wipes her hand across the smooth granite plaque.
She doesn’t keep track of how much time she spends on her battle for change in Japan. In the beginning, the family wasn’t sure about going public with Kelly’s death. But since they did, she hasn’t slowed down. “I’m basically just like the stereotypical mother whose child has died and they go out and they work for the cause to try to keep other people from doing the same thing. I just feel like I have to do this, I can’t let anybody else have to go through this … Instead of crying, I fight ... That’s all I’m gonna do, I’m not gonna stop until I can get some kind of solution to this problem.” She has an enormous battle on her hands.

In the 1950s, throughout much of the Western world, the ‘deinstitutionalisation movement’ saw a push towards the closure or downsizing of psychiatric hospitals, and the development of community-based mental health services. In most OECD countries, the number of hospital beds has dropped steadily since the 1970s. But in Japan, the number has actually risen.
In 1958, the Japanese government passed a law allowing a lower staff to patient ratio in psychiatric hospitals than in general hospitals. The law allowed facilities to increase bed numbers without incurring the cost of hiring extra staff, fuelling the expansion of private psychiatric hospitals.
Today the low staff to patient ratio law (one doctor per 48 patients, and one nurse per five patients) remains in place, meaning a relatively small workforce is responsible for a large number of patients. Tsukuba University professor of psychiatry Tamaki Saito identifies this as a major cause of high restraint use in Japan. He also believes that many mental healthcare workers prefer to restrain patients because they fear being held responsible for their injury or suicide, and that patients are being restrained upon admission to hospitals - almost by default. “I think body restraint is a routine order when accepting in-patients.” Despite being legal only as a last resort method, used for short periods of time when no alternative is viable, the number of patients restrained has more than doubled in Japan, from around 5000 in 2003 to 12,528 in 2017.
Saito believes this is completely unnecessary, and that the number of cases of restraint could be reduced to fewer than 100 if patients were assessed more carefully upon admission to hospitals.
Though change is slowly coming to Japan, with psychiatric hospital bed numbers and average length of stay falling very slightly in the last decade, Saito, like journalist Yukiko Okuma and others, believes that the Japan Psychiatric Hospitals Association and its affiliated hospitals is partly to blame for a lack of any meaningful reform, or a stronger push towards deinstitutionalisation: “Staff and directors of private hospitals are afraid of losing their beds and their incomes. The number of patients is decreasing now, so they cannot run their hospital,” Saito says. “I think many Japanese psychiatric hospitals will go bankrupt in the next 10 years because of the decreasing number of inpatients. They are afraid of reducing beds, so they resist moving to a community care system.”
In the 1980s, the Asahi Shimbun newspaper revealed that two patients at a Japanese psychiatric hospital were beaten to death by staff wielding metal bars. The murders drew outrage among the people of Japan and international criticism of the country’s mental health law, which led to reform. In Japanese, the word for this type of change driven by external pressure, is ‘gaiatsu’. Saito and Okuma believe it is gaiatsu that will again lead to reform of the current system.
Patrick Savage also holds out hope that gaiatsu will lead to change within a system that has caused him, his family and many others in Japan so much pain. “Japan doesn’t change by itself, it changes by pressure from the outside. So the fact that Kelly was a foreigner in Japan, I think, [makes] it a lot more likely that things would change.”

On an overcast, spring morning, he stands outside Yamato psychiatric hospital - a multi-storey, grey and foreboding building somewhere in the urban sprawl between Tokyo and Yokohama. On the hospital’s website, blossoming cherry trees surround the building, but on this day, they are nowhere to be seen. Helicopters and crows fly overhead, while pedestrians and cyclists pass by. Do they know what goes on inside that big grey building, and the thousand other psychiatric hospitals throughout Japan?
Patrick does now, though he wishes he didn’t. “It needs to stop,” he says. He hopes Kelly’s legacy will make that happen.
Where to get help:
Skylight: 0800 299 100 / Skylight is a support organisation that specialises in grief, loss and trauma.
Heartsong: a Skylight facilitated group for parents in the Wellington region, who have been bereaved by the loss of a child. 0800 299 100
1737: Free call or text 1737 any time to speak to a trained counsellor, for any reason.
Depression Helpline: 0800 111 757 or free text 4202
If it is an emergency and you feel like you or someone else is at risk, call 111.
Reporting Susan Strongman
Executive editor Veronica Schmidt
Research and translation Hiroko Aihara
Additional translation Yumi Nagafuchi
Videography and photography, Japan Luke McPake
Videography and photography, Wellington Rebekah Parsons-King
Design Luke McPake
Video edit and post-production Luke McPake
Bumper car footage Charmaine Lam
Art direction Dave Wright
Development Van Veñegas
Made with the support of the Asia New Zealand Foundation
